In many developing countries, public sector absence is both common and resistant to reform. One explanation for this is that politicians provide public jobs with limited work requirements as patronage. We test this patronage hypothesis in Pakistan using: (i) a randomized controlled evaluation of a novel smartphone absence monitoring technology; (ii) data on election outcomes in the 240 constituencies where the experiment took place; (iii) attendance recorded during unannounced visits and; (iv) surveys of connections between local politicians and health staff. Four results support this view. First, while doctors are present at 42 percent of clinics in competitive constituencies, they are present at only 13 percent of clinics in uncompetitive constituencies. Second, doctors who know their local parliamentarian personally are present at an average of 0.727 of three unannounced visits, while doctors without this connection are present at 1.309 of the three visits. Third, around 40 percent of inspectors and health administrators report interference by politicians when they try to sanction doctors. Fourth, the effect of the smartphone monitoring technology, which almost doubled inspection rates, is highly localized to competitive constituencies. Last, we find evidence that program impact is in part due to the transmission of information to senior officers. We test this by manipulating the salience of staff absence in data presented to officials using an online dashboard. These effects are also largest in politically competitive constituencies. Our results have implications for the study of bureaucratic incentives in fragile states and are potentially actionable for policymakers trying to build state capacity.
That is the abstract of a paper titled “The Political Economy of Public Employee Absence: Experimental Evidence from Pakistan.”
****
“random read” is a new series of posts on haba na haba highlighting research papers using experiments. Feel free to email me any you find interesting that could be part of the series!
on being diagnosed with cancer
Today Oliver Sacks — a neurology professor at NYU and a prolific writer — wrote an op-ed for the New York Times, “My Own Life,” on learning that he has terminal cancer. Lots of friends are sharing it on Facebook, drawing quotes they find moving. The passage that stuck most with me was:
I feel intensely alive, and I want and hope in the time that remains to deepen my friendships, to say farewell to those I love, to write more, to travel if I have the strength, to achieve new levels of understanding and insight.
This will involve audacity, clarity and plain speaking; trying to straighten my accounts with the world. But there will be time, too, for some fun (and even some silliness, as well).
I feel a sudden clear focus and perspective. There is no time for anything inessential. I must focus on myself, my work and my friends.
I know this feeling. Perhaps a bit more than I’d like. On the day before Thanksgiving, I was diagnosed with cancer. To be more specific, I was diagnosed with Chronic Myeloid Leukemia (CML).

A small, hypolobated megakaryocyte (center of field) in a bone marrow aspirate, typically of chronic myelogenous leukemia. Image courtesy of Difi Wu, shared with CC license via Wikimedia Commons
CML is not terminal cancer. I’m not dying. Not much more than the rest of you, anyway. (Maybe even less.) As we wrote in the family Christmas letter this year, “If one has to have cancer, CML is the best one to get (Kim’s exceptional taste appears to extend to health ailments!).”
There is a treatment for CML — in fact, there’s more than one treatment option. I have elected to take a daily pill. I have been taking it for just over two months now, and all things going well, I will take it every day for the rest of my life. I just checked in again with my oncologist a week ago and my prognosis is pretty great. My body is already responding to the treatment and I’m not experiencing strong side effects from the medication.
But a couple of months ago, I was a mess. Every time I remembered “I have cancer”, I thought about my two-year-old. My seven-year-old. My husband. My best friend. And thinking about my mom really did a number on me. Recalling it now causes my eyes to well up.
But back to the passage in the op-ed by Sacks. When I told a friend and colleague about my diagnosis, she encouraged me to scale back on work. (She was diagnosed with cancer and tough as she is, the cancer and the treatments really wiped her out. She is in remission now.) After suggesting I scale back, she promptly said that I should do what I wanted, that everyone is different and maybe working full-tilt was actually the best option for me. That maybe I’m the kind of person who would benefit from just moving on as usual. She said that having cancer did not make her a better person or make her reconsider her life.
My experience was different. Like my friend, I don’t think that cancer has made me a better person, but I have reconsidered my time. Sure, my diagnosis is not on the same level of Oliver Sacks. But my diagnosis clarified for me how I want to spend the time I’ve been gifted with. For better or worse, there are plenty of things I’ve decided I have no time for. And there are fewer things I find worth being away from my family for.
Monday mbalimbali: the week in images
- Photos that gave Americans their first glimpse of Apartheid in 1950

- Mobutu’s ruins in Gbadolite

- Putting the New England snow in perspective

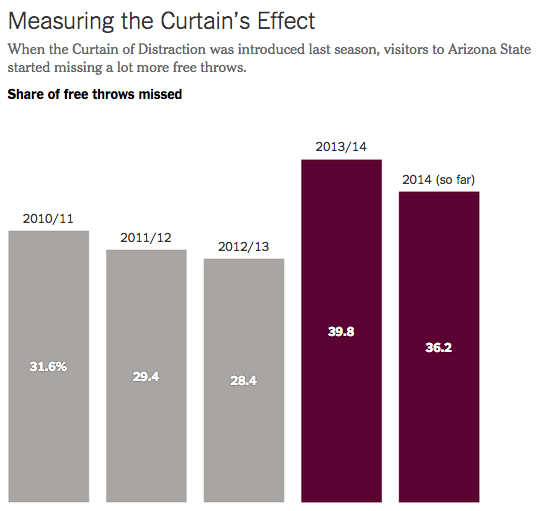
- Why I’m concerned about the Wednesday UCLA game at ASU.
- Making light of the recent brawl in South Africa’s parliament.
Monday mbalimbali: Measles edition
- A Bard college student who “tested positive for measles was contagious when he boarded an Amtrak train last Sunday and potentially exposed thousands of travelers to the infection.”
- According to the CDC, as of January 28, there were 84 people in 14 states in the U.S. reported to have measles.
- On the causes of the outbreak, some are blaming anti-vaxxers, a derogatory, catch-all term for people who choose — despite the litany of evidence that vaccines are safe and effective — not to vaccinate themselves or their children.
- Others are pointing to overseas travel as the major cause of the outbreak.
- Naturally, Vox.com is hedging its bets, saying it could be both anti-vaxxers and overseas travel.
- In the wake of the outbreak, Bard College is reportedly requiring students show proof of vaccination, get vaccinated, or stay off campus for 21 days.
- Beyond the Bard campus, doctors are refusing to see children whose parents refuse vaccination.
Monday mbalimbali
- Zambia has elected a new president, Edgar Lungu, of the ruling Patriotic Front party.
- Indian Prime Minister Narendra Modi is married, but it seems he hasn’t spoken to his wife in years. She’s waiting for his call.
- In the latest IMF/Ebola news, Guinea President Alpha Conde has asked the IMF to cancel its debt to aid its recovery from Ebola.
- Secretary of State John Kerry flew to Lagos and met with Nigerian President Goodluck Jonathan and his opposition candidate in the upcoming February 14th elections, Muhammadu Buhari.
- Last year, DC think tanks held more than 150 events on the Middle East where only men spoke.
- A good reason to switch to Lyft from Uber.
- Best headline of the week: Breast implant leak delays Rep. Alan Grayson’s wife’s bigamy trial.
- Finally, some frivolity. I don’t speak Italian, but I think this is science. At least, it involves a few things I like: Nutella, Coca-Cola and condoms.
Monday mbalimbali: #MalawiFloods edition
My new year’s resolution was to at least post weekly to haba na haba,* reviving the “mbalimbali”** posts — what others might call “miscellaneous” or “links I liked”.
This Monday’s edition focuses on the floods in Malawi, which began earlier this month and continue to wreak havoc, particularly in the southern part of the country.
- The BBC estimates 200,000 Malawians have been displaced by the floods.
- Al Jazeera reports Malawians are angry at the slow response to the floods.
- The Daily Maverick (a South African newspaper) reports 170 have died.
- A project coordinator with Medecins Sans Frontieres (MSF, aka Doctors Without Borders) describes what he saw in the most southern district of Malawi (Nsanje) from his perch in a helicopter.
- An earlier MSF report estimated 20,000 Malawians were completely cut off from receiving food aid.
- On Tuesday, January 13, Malawi President Peter Mutharika declared a state of emergency.
- The most reliable, up-to-date source of information from the Malawi government is their Facebook page, where there have been (at least) daily updates.
- The International Charter — a multinational collaboration of space agencies in Europe and Canada — has used multiple radar satellite images to create detailed maps of the flooded areas in southern Malawi (and northern Mozambique).
- A lot of the photos I’ve seen are devastating. Here are just a few that folks have posted to Twitter:
________
* Clearly, as we are almost three weeks into the new year, I’m already failing at keeping this resolution.
** In Chichewa/Chinyanja, mbalimbali has a number of meanings/translations to English. In addition to meaning “around (the sides)“, it can also mean “various” (as could siyanasiyana).


